|
Impact of defaulting to single-lumen peripherally inserted central catheters on patient outcomes: An interrupted timeseries study. An intervention involving setting PICC default orders to single-lumen devices, establishing criteria of when multi-lumen PICCs are appropriate, and provider, nursing, and pharmacy education resulted in significant decrease in inappropriate PICC use as well as an overall increase in single lumen PICC use.Less lumens-less risk: A pilot intervention to increase the use of single-lumen peripherally inserted central catheters. This article provides a detailed summary of the available evidence for detecting, identifying, and treating upper extremity deep vein thrombosisīozaan D, et al. Three-quarters of thrombotic events occurring in veins of the upper extremity are due to the presence of intravenous catheters. 
Intravenous catheters cause endothelial trauma and inflammation that often progresses to venous thrombosis.Catheter-related upper extremity venous thrombosis. A multi-modal intervention based on MAGIC resulted in a modest decrease in inappropriate PICC use.Improving PICC use and outcomes in hospitalized patients: An interrupted time series study using MAGIC criteria. Every 5% increase in single-lumen PICC use would prevent 0.5 PICC-related central line-associated bloodstream infections and 0.5 PICC-related deep vein thrombosis events, while saving $23,500.Infection Control & Hospital Epidemiology 2016 Limiting the Number of PICC Lumens to Improve Outcomes and Reduce Cost: A Simulation Study. Application of MAGIC by clinicians and providers within intensive care areas may assist hospitals in establishing reliable access, improving outcomes, achieving infection prevention goals and reducing burden of thrombosis MAGIC provides guidance on assessing the appropriateness of PICCs and other vascular access devices for the intensive care patient.Making the MAGIC: Guiding vascular access selection for intensive care - a summary of Michigan Appropriateness Guide for Intravenous Catheters (MAGIC). Use of central venous catheters (CVCs) was strongly associated with risk of UEDVT 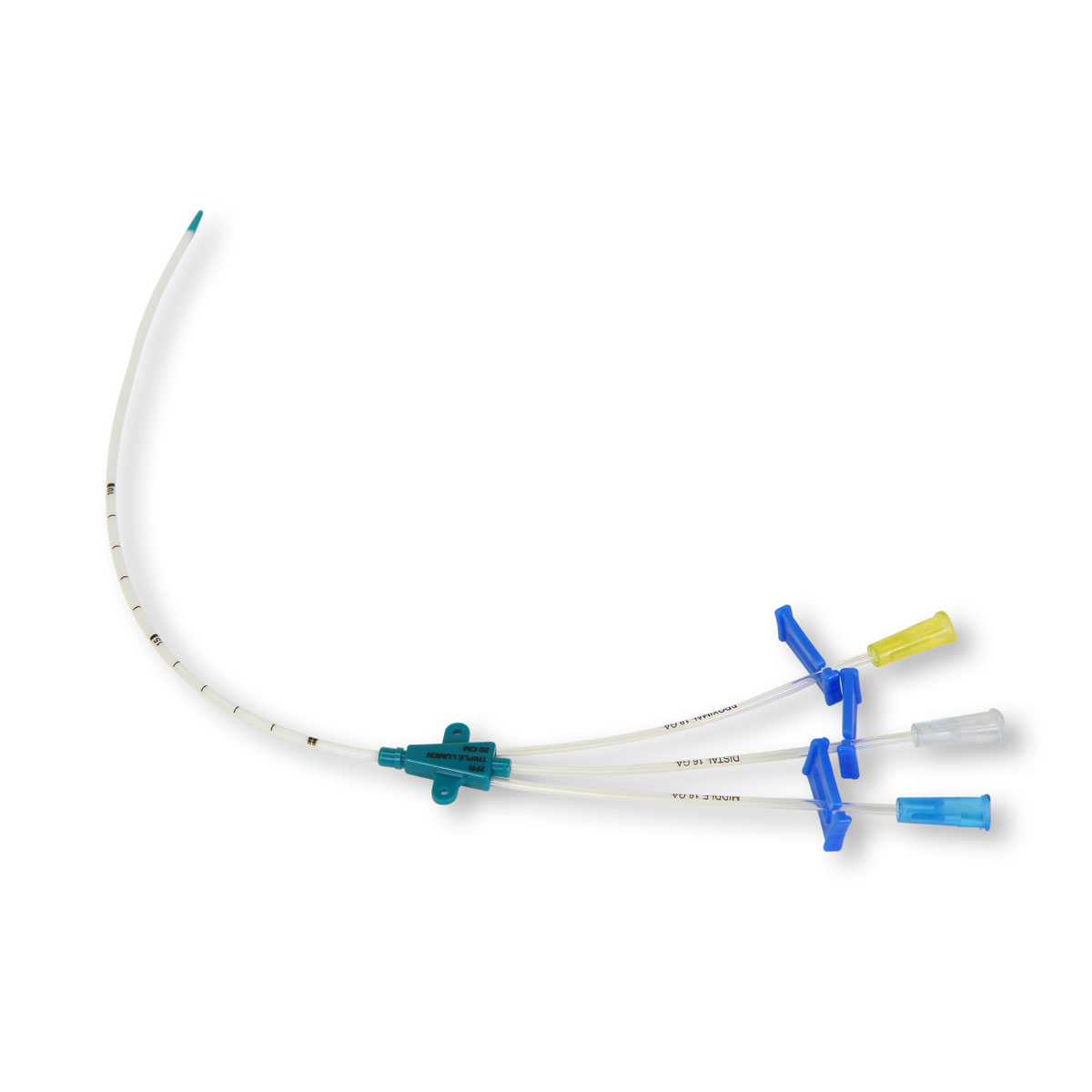 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
